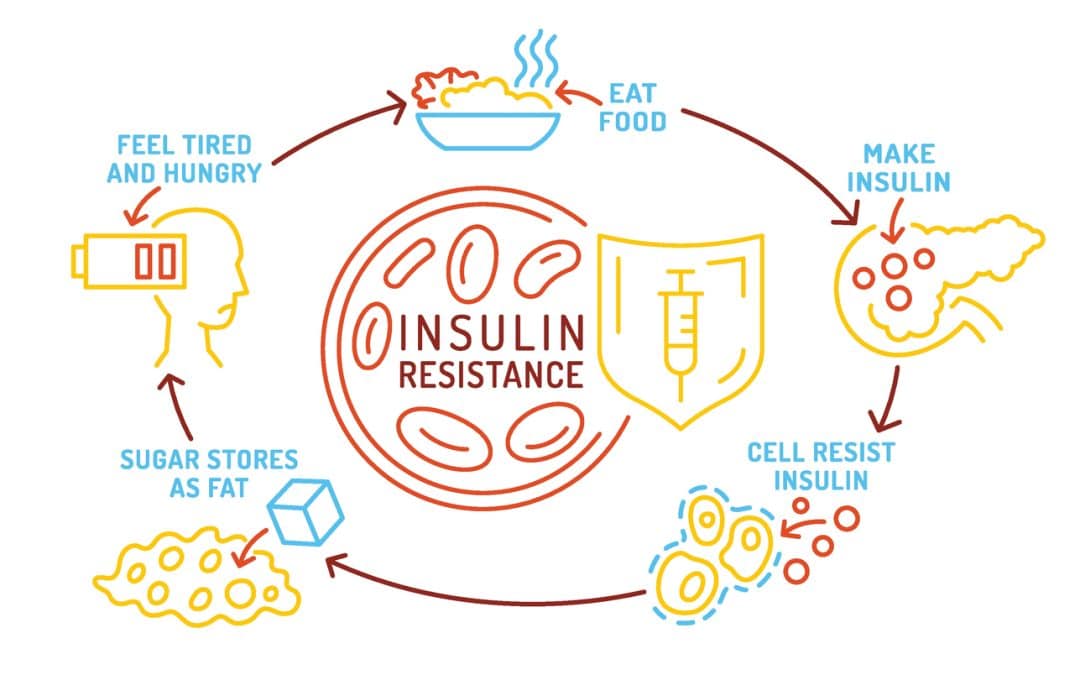
One of the things we talk about often in our office is a monster of a problem called insulin resistance—and for good reason. It's one of the most common yet overlooked root causes of issues like fatigue, stubborn weight gain, brain fog, hormone imbalances, and more....